Top management issues for designing or upgrading a clinical lab
By Gary Tufel
Designing, upgrading, and choosing the right instruments for a clinical lab are complicated tasks. Even for experienced laboratory directors and managers, it isn’t always apparent how such processes should be conducted, or how a lab should go about ensuring that its specific needs are addressed.
When designing a new lab that has never been inhabited, lab directors and managers should create one that will allow them to easily adapt with the times and technology, says Lonnie D. Stallcup, Jr, BS, MT, continuous process improvement manager at the Laboratory Alliance of Central New York LLC, Syracuse, NY.
“Many labs have been set up with permanent casework,” Stallcup says, “and while that design may make sense at its inception, as new technology comes in, it may not support the workflow.” Furthermore, he adds, lab directors and managers should consider every instrument and workstation that must go into the laboratory to ensure that each workstation has the required data, electrical, and plumbing connections for staff to complete their jobs efficiently.
As for upgrading a clinical lab, many of the same rules apply, but one could reasonably assume that this is a more difficult challenge, Stallcup says. That’s because the laboratory will need to continue providing uninterrupted care to patients. Therefore, it is imperative that the director or manager have a well-developed plan for upgrading the laboratory.
“Basically, the amount of growth the laboratory expects over the next 5 to 10 years—in both current test methods and new technologies—will affect the size of the needed space,” says Rodney G. Day, MS, MT(ASCP), SC, senior laboratory consultant at LGP Consulting Inc, Wood River, Ill. “Additionally, directors must understand the value of Lean principles on the design and cost of upgrading, and make sure to meet all safety codes and regulatory standards for accreditation.”
For Kenneth McWilliams, MT(ASCP), MBA, a process consultant with Beckman Coulter Inc, Brea, Calif, working closely with facilities, maintenance, and construction contractors is critical. It’s essential to have them on board.
“Plumbing for drains can be one of the more challenging aspects of lab design, as drains are fixed into the floors,” says McWilliams. “Labs located in basements or bottom floors that do not have access underneath their floor can incur higher costs for relocating drains. However, ensuring that there will be adequate power, HVAC, high-quality water, drainage, and additional IT connections are also very important.”
DOCUMENTS, CHECKLISTS, AND GUIDES
Day says there are numerous documents on laboratory design that directors and managers should consider. “These are generally documents that present safety regulations or standards (such as those compiled by the American National Standards Institute), documents providing guidance and suggestions from professional organizations (such as the American Association for Clinical Chemistry, or AABB), or published sources from subject matter experts presenting concepts related to Lean processing in clinical labs. Publications in the last group often include significant detail about planning to optimize a lab’s walking distances, workflow, movement of pieces, and so on, using such quality systems strategies as ’kaizen’ (the practice of continuous improvement) and ’kanban’ (a scheduling system for Lean and just-in-time production).”
McWilliams says Beckman Coulter uses project managers (PMs) to help customers prepare for installing new automation equipment. Since every lab is different—and so is their automation system—there is no “cookie cutter” document that will help with everything. PMs help customers make sure that everything is accounted for, and develop a timeline of the items that need to happen and in what order.
Ironically, says Stallcup, he can’t really say that he’s operated off a standardized checklist or guidance document. “When my company introduced Lean into its culture, we invited a consultant to guide us through our first Lean project. In future projects, we drew upon the methods provided by the consultant, but we also went on to develop our own methods.”
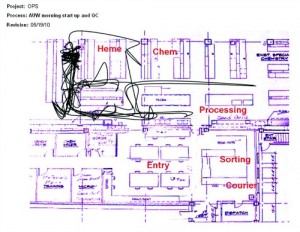
A point-to-point “spaghetti” diagram, showing a clinical laboratory’s morning routine and quality control activities before the adoption of Lean processing. Image courtesy Laboratory Alliance of Central New York.
For each of its Lean projects, Laboratory Alliance appoints a Lean team that incorporates a mix of management and front-line staff. “We have found great success with involving staff in the planning, as they not only provide valuable input but are then also better engaged to support the changes introduced by Lean,” says Stallcup. A large part of the Lean team’s responsibility is to develop many potential lab designs, and present those designs to the stakeholders for consideration.
“To assist us in this endeavor, we utilize Microsoft Visio to develop the various designs,” says Stallcup. “However, coming up with potential layouts is really the easy part. Once we determine the final layout for each lab, we plan every last detail for the transition of the lab. Utilizing something as simple as Microsoft PowerPoint, we are able to ‘animate’ each step of the transition. In doing so, we can better predict the various needs for each step.”
AUTOMATED SYSTEMS GUIDE DESIGN AND EQUIPMENT SELECTION
When selecting equipment for a new or upgraded clinical laboratory, directors and managers should be mindful of the types of technology incorporated into prospective systems, and how various technologies may have different clinical, operational, and financial affects on a hospital. “Much improvement in efficiency and productivity can be gained from the analyzers themselves; especially if there is a higher level of technology associated with them,” says Nilam Patel, MT(ASCP), SH, senior product manager for automated solutions at Sysmex America Inc, Lincolnshire, Ill. “For example, getting six-part differentials with immature granulocytes, immature platelet assessments, and reticulocytes on the first pass will reduce potential manual procedures and provide a higher level of clinical information for physicians to monitor patients.”
Reruns and reviews are often the most time-consuming part of testing, says Patel. Automating the ability to minimize such interruptions to workflow is often more important than a system’s time to first result. “Laboratories will also want to consider the ‘track record’ and reliability history of vendors’ products, and their ease of use to address various skill levels in the laboratory. System flexibility and scalability will help laboratories plan for future growth while ensuring that an overbuy or underbuy decision is not made.”
According to McWilliams, criteria to be considered should include not only a system’s speed, but also its overall throughput. Measured by speed alone, a centrifuge that can spin down a sample in 5 minutes should be able to perform 12 runs per hour. But the instrument’s load and unload time is also critical. “We look at the mean time for our existing systems to show the average time through the centrifuge,” says McWilliams.
The sheer size and speed of an automated system should not be the only criterion for choosing among several candidate systems, says McWilliams. “What’s the point of selecting an automation system that does not do all that you need it to do? For example, the purpose of automation is to automate a process or processes, not to create two new processes, such as one process for routine tests and another for stat tests. An automation system should accept any priority instruction.”
Even tube size can be a significant consideration affecting equipment selection, says McWilliams. “While having the ability to handle multiple tube sizes is nice, the best solution is standardization. This helps not only in workflow, but in ordering, costs, and storage.”

During a laboratory update, two instruments undergo validation. Temporary electrical lines have been fed from the ceiling; blue tape on the floor marks the future location of the automation line and instruments. Photo courtesy Beckman Coulter Diagnostics.
Space constraints must also be considered, says McWilliams. In many hospitals, laboratories reside near the bottom of the institution’s priorities, and lab directors and managers have been unable to demonstrate to administrators that lab expansion can increase a hospital’s return on investment. In such instances, labs may be compelled to settle for whatever lab equipment fits their existing space, instead of lobbying for expansion that would enable them to improve their business performance. “Institutions should invite input on space constraints from lab techs as well as from other departments that work with the lab and depend on it,” says McWilliams. “For many institutions, the aging population of lab techs, combined with financial constraints and increased workloads, is creating a tendency toward lab consolidation. To retain laboratory specialists, institutions must maintain a delicate balance. The alternative is to make the difficult decision to go to core labs.”
When selecting software systems to help in lab design, lab directors and managers should choose a system that is relatively easy to use and will yield accurate information. “While Microsoft Visio is a nice program to use, some labs may find the software to be quite costly, depending upon how many licenses are needed,” says Stallcup. “Other products are available for free and can be used to develop the same information. The system needs to allow users not only to capture the current lab and the future lab, but to demonstrate how the transition from the current to the future will occur.”
Although no entirely automated programs are available to assist in lab design, says Day, use of common software programs such as Visio can help with drawing to scale, checking distances, and calculating walking time, waiting time, and other factors. “A higher level would be to use simulation software that enables planners to model the physical environment and corresponding lab processes, and to run projections for areas such as throughput, waste, waiting time, and so on. Professional-level software, such as Witness, is pretty expensive. But it can be used by laymen, rather than mathematicians, to develop Windows-based simulation models.” Common factors generally considered by such programs include cost, service, value, need, and capacity.
ACCOMMODATING FUTURE GROWTH
When seeking to plan for future growth, Day advises, lab directors and managers should estimate how much the lab expects to grow over the next 5 years as a minimum, and should consider not only increases in volume, but new technology as well.

Strategic positioning of this movable workstation between two chemistry analyzers allows easy access to instruments for loading and results review. Photo courtesy Laboratory Alliance of Central New York.
When planning for the future, says Stallcup, lab directors and managers should try to anticipate and address any changes that could potentially affect the laboratory. “If we know reimbursements in the future will be less, then we have to prepare for how to use our staff more efficiently,” he says. “This may even mean that we have to consider better automated testing methods.”
Based on calculations of future reimbursement and staffing, says Rita Romano, director of the operations center at the Laboratory Alliance of Central New York, it may even be more cost-effective for some institutions to consider outsourcing certain types of testing.
McWilliams agrees that it is critical for lab directors and managers to look at both the past and potential future growth when charting their course. “The key is to look ahead at not just what your current problems are, but at any foreseeable problems or concerns,” he says. “A medtech population that is reaching retirement age, along with a decline in the number of medtech schools, means that either more automation will be needed or hiring more lab assistants will be necessary.”
“Labs shouldn’t wait until the last minute, or buy equipment anticipating that things will remain the same,” McWilliams says. “Decisions must be based on hard data about workflow, volume, and peak activity times.”
Standardization is also a desirable part of this process, especially for reference labs that receive different tube sizes from various sources, each requiring a different centrifuge. “Becoming a Lean lab—one that aims to perform tests and deliver results in the most efficient way in terms of cost, or speed, or both—requires an increase in efficiency and in the quality of results, and a decrease in laboratory time and expense.”
STAFF RECRUITMENT AND RETENTION
Recruiting and retaining professional staff at the appropriate education and skill levels has become increasingly difficult, and the majority of labs nationwide are now experiencing some form of staff shortage.
“It has been estimated that even if all of the laboratory programs in the United States were filled to capacity, there would still not be enough new graduates to meet the needs of medical laboratories,” says Stallcup. “If a laboratory can, it should serve as a host site for both medical laboratory scientist and medical laboratory technician students to complete their clinical rotations. Doing so affords the lab the opportunity to dazzle potential employees, and also allows the lab to screen students and determine if they are a perfect fit.”

In this rapid response lab, a coagulation analyzer and a urine analyzer have been placed close to one another to permit efficient use of one technician’s time for processing specimens. Photo courtesy Laboratory Alliance of Central New York.
Unfortunately, serving as a host site for clinical rotations may not solve all staffing woes, and labs may need to undertake additional approaches. “At one point, I worked with others in my company to identify nontechnical staff members who we felt would be excellent technicians or technologists, and offered them an opportunity to become technical staff,” says Stallcup. “Those who accepted completed academic training online while completing their clinical training in our lab. They continued to work as nontechnical members until completing the necessary training. We then elevated them to technologist or technician status.”
“Lab personnel must meet the various standards of education and skill necessary for fulfilling regulatory requirements,” says Day. “Beyond this, lab directors should ensure that their staff meet appropriate education and training requirements for the various tasks they perform, and that tasks at different levels are clear. In too many labs, medical technologists function no differently than medical technicians or lab assistants. This leads to issues in retention, recruitment, and setting appropriate salary levels. Ensuring job satisfaction of professional lab workers goes a long way in retention, including recognition of the worker’s value to patient care.”
“Neither traditional nor nontraditional routes of recruitment will produce professional staff as quickly as we need them,” says Stallcup. It is therefore imperative that lab directors and managers look at the work being completed by technical staff and determine whether any of that work can be redirected to nontechnical staff. “In doing so, we can ensure that we are using our lab professionals as efficiently as possible.”
PREVENTING OVERBUYING AND UNDERBUYING
Projecting future growth enables lab directors and managers to avoid reaching complete saturation of their equipment before an existing leasing contract is up or, if purchased, before they have fully depreciated the instruments.
“Most labs are looking at ways to increase the volume of tubes coming into their lab, either by luring in outreach or offering more testing in-house,” says McWilliams. “With the integration of hospitals into larger health networks, some labs are seeing consolidation into larger core (or main) labs that perform most esoteric or specialized testing, while retaining only the minimum amount of stat or necessary testing at local sites.”

Wheeled tables enable instruments to be moved if workflow needs change. Photo courtesy Laboratory Alliance of Central New York.
Another factor that influences what equipment a lab should buy is where the lab will place the equipment. “How many labs have put equipment somewhere simply because that’s where it has always gone, or because it belongs to someone’s department, or even because that was the only place it would fit?” asks McWilliams. “Using Danaher Business Systems techniques such as spaghetti diagramming to depict workflow can help a lab realize how inefficient its current layout is.
“Equipment should be placed in a way that enhances workflow. With the decline in the number of clinical laboratory scientists and medical technologists coming into labs, and the need for labs to become more flexible with their staffing, it will be necessary to break the traditional boundaries between departments, and to lay out equipment in a way that helps get more work done with fewer steps,” adds McWilliams. “Saving a few steps of walking increases the happiness of those in the lab, and also saves the lab money by making its employees more efficient.”
Even when instrumentation has already been selected, project managers in charge of upgrading a facility can face tough decisions. “We still had considerations to make regarding the removal of casework and replacement with mobile workstations,” says Stallcup. “We budgeted for each of our projects and strived to operate within the confines of the budget. Fortunately, since our group is a network of labs, our buying power was a bit better, and we were able to find affordable furniture that helped us achieve our goal. Our purchases were never frivolous, but were always aimed at improving patient care.”
It’s essential to define customer and patient needs for turnaround time and how often tests must be performed, says Day. “With major instruments, all the vendors can run simulations for turnaround time and capacity, but care must be taken not to use only theoretical maximum throughput, but what can be expected in the planner’s lab in reality,” he says. “Lab directors must be careful about their back-up requirements—the tests that must always be available, even if some instruments are down. All vendors’ recommendations for sizing should be checked with current customers of that vendor.”
EQUIPMENT NEEDS BY CLIA RATING AND SPECIALTY AREA
Romano says that the lab directors and managers of each specialty area should conduct an assessment to ensure that the equipment purchased for their areas provides the highest throughput while optimizing staff efficiency. Each laboratory’s assessment will be unique, based on its patient mix, provider needs, staffing, and budget. (For more information, see the companion article, “Professional Consultants Tackle Improvement.”)
“Clearly, some types of equipment are required for high-complexity tests that would not be needed for moderate-complexity tests,” says Day. “Almost all specialty areas have their own instrument requirements, except for general items like centrifuges, but even these are also specialized for some sections.”
In any case, says Day, an instrument’s CLIA rating may be less important than several other factors for making a final equipment selection. The equipment’s use, capacity, and throughput are important factors. Also important is the overall value of the equipment, as indicated by its total cost of operation (instrument, reagents, maintenance, waste, personnel), measured incrementally based on workload.
DATA TO GUIDE PURCHASING DECISIONS
Among sources that can guide equipment purchasing decisions, Day advises the use of instrument vendors, consulting services, independent workflow consultants, comparisons of instruments in trade and professional journals, and checking with current users of instruments in labs of similar size.
According to McWilliams, hard data offers the best guide for purchasing decisions. A great place to start is with data from a laboratory information system (LIS) showing the volume of tests currently being reported.
“Don’t assume you know what your volume is. Look at the true numbers. But more than just the numbers, look at when and how the tests are arriving rather than just an average of daily volumes,” says McWilliams. “A lab may have high peaks during one part of the day and then slower times at others. In a hospital lab where turnaround time is critical, managers must plan to have enough throughput to handle the peak times, not just the average daily volume.
“This may seem like overkill during a lab’s slower times, but having the capacity to handle peak volumes could be critical,” McWilliams adds. “If you are unable to do this, then explore ways to adjust the timing of when specimens arrive in the lab. Think about more courier runs to bring in samples in smaller batches. Be creative.”
HOW AND WHEN TO PURCHASE EQUIPMENT

During a laboratory update, instruments and components shipped into the lab are stored until needed for installation. Photo courtesy Beckman Coulter Diagnostics.
Whenever a major instrument acquisition is to be budgeted, says Day, purchases should be made as soon as feasible. Because of long capital expense budgeting cycles, in many hospital settings instruments may be purchased 1 to 2 years before installation.
The need for instruments to be replaced may become apparent by measuring their current performance. “If an instrument in our lab is down, we actually track the downtime,” says Stallcup. When an instrument has too much downtime, the lab should consider replacing it. But for hospital administrators, the best case of the need to upgrade instrumentation is always accompanied by data. Turnaround time data may be one of the best ways to prove the need for better instrumentation, as it directly affects patient care and client satisfaction.
“Our information systems team has been essential in helping us to pull such data from our LIS and present it using Crystal Reports software,” says Stallcup. “Obviously, if directors or managers suspect a deficiency, there is no time like the present to begin generating the necessary data. However, just as in driving, it is important to keep your eyes on the road at all times. Therefore, key performance indicators should be identified and monitored over time to ensure that the system is in balance.”
McWilliams notes that this kind of data should be able to be pulled out of most LISs. But some systems are more user-friendly than others. Some provide exactly the data that is needed, while others are cumbersome to use or require help from outside the lab—and may still lack the necessary information.
Another problem with using only data from the LIS is that it only shows past data, adds McWilliams. Beckman has developed a partnership with hc1.com to provide real-time data. “Past performance is necessary to understand past volumes and turnaround times, but knowing that there was a problem a day, week, or month after the fact is not good enough to fix the problem. Having real-time data lets labs know when they are having a problem, so that they can take care of it more quickly.”
Following up on the solution to the problem and making sure that the solution has worked long-term are equally important steps, says McWilliams. “Using techniques such as a problem-solving process to conduct a root cause analysis is critical. Don’t just put a Band-Aid on the problem when stitches are needed.”
In this area, outside process consultants can be a big help, offering a fresh perspective about a lab’s challenges and questioning methods—and offering solutions—all based on hard data.
Even where lab volumes may be high, many labs still have turnaround times that are less than optimal. But looking at such factors as the number of techs in the lab at peak testing times, or whether instrument settings and maintenance schedules are optimized, can vastly improve results and efficiency, says McWilliams.
WHO TO INVOLVE IN PURCHASING DECISIONS
Making the assessments and decisions necessary to create or upgrade a clinical lab can involve a large number of stakeholders. Day suggests that the team should include the lab director from a medical standpoint, but with full coordination with the lab manager from a business standpoint, section lab technologists from a need and use standpoint, and appropriate finance staff and buyers. For high-priced systems—especially total lab automation systems—the involvement of a hospital’s chief of staff or medical or surgical department chiefs may be required to ensure that lab equipment purchases receive priority over the needs of competing departments.
In the case of Stallcup’s Lean team, purchasing recommendations were presented to the lab directors, managers, and supervisors. “These folks had a vested interest in what we were trying to accomplish, and they were able to offer timely advice about whether our approach would work.”
More and more, labs are getting involved with the C-suite, and sometimes the ultimate purchasing decision is not made in the lab, says McWilliams. But that doesn’t necessarily mean that labs lack a say in what equipment they ultimately lease or purchase. Labs that can show how acquiring new equipment will enhance their performance, lower operating costs, and improve quality will have a head start on convincing hospital administrators. But to clinch the case, labs may also need to show how a revitalized and re-equipped lab will improve their organization’s return on investment.
Every lab is cost conscious, but it is not always easy to see cost benefits in improving quality, safety, and satisfaction with patient care. “I would caution everyone not to allow these qualities to be undervalued,” says McWilliams. “As reimbursement policies are changing, with hospital performance and patient satisfaction playing a bigger role than ever before, it is imperative that lab directors and managers know how to explain improvements in the lab and how they are affecting these metrics.”
Gary Tufel is a contributing writer for CLP. For further information, contact CLP chief editor Steve Halasey via [email protected].