Choosing the correct individualized treatment for breast cancer depends upon determination of receptors for estrogen, progesterone, and HER2. The gold-standard method of doing this is currently immunohistochemistry (IHC). However, in 5% to 10% of cases such testing of tumor tissue can produce false-negative or false-positive results, with serious consequences for the patient concerned.
In a joint interdisciplinary project, researchers from the Medical University of Vienna have now demonstrated that diagnostic certainty can be significantly increased by a new investigation technique: namely, by checking the gene expression of the receptors on a gene chip, and then collating all the data in a mathematical model to derive an overall result.
If one or more receptors that drive breast cancer is detected, then antihormonal therapy is the correct and most-effective treatment. It inhibits the disease process and causes the receptors to diminish. Comparatively stressful chemotherapy with its many side-effects is not necessary, although it could be used without any life-threatening consequences. However, if IHC shows that none of the receptors is present and that breast cancer has developed without their ‘drive,’ then chemotherapy is usually used.
The problem arises when IHC has produced a false-positive result due to a measurement error—that is, no receptors were actually present, despite the test results, causing hormone therapy to be given erroneously. “In this case the error can be life-threatening,” says Wolfgang Schreiner, PhD, of the institute of biosimulation and bioinformatics at the Medical University of Vienna.
To increase certainty in determining receptor status, Vienna bioinformaticians looked at data from 3,241 patients from 36 clinical studies and developed a gene model for each receptor. “Before forming the protein material for the receptor, the gene first produces an RNA copy, a sort of ‘blueprint’ for the receptor,” Schreiner explains. “Using the gene chip, we can determine whether this RNA copy is present in the tumor tissue. That is an important marker.”
At the same time, so-called co-genes were identified in each case, these being the second-commonest genes associated with receptor formation. The information from IHC and from expression of the receptor genes and co-genes was fed into a robust mathematical model that served to eliminate false results fairly accurately.
“One could continue this series indefinitely,” says Schreiner. “We could now feed additional omics data sources into our analysis, one after the other, until we have reduced false-positive or false-negative results to virtually zero. We will then have certainty.”
In the future, such a fusion of omics data—molecular biological data seen from various angles—will enable scientists to keep increasing precision in diagnosis and treatment, in keeping with the spirit of personalized medicine. “Our task lies in utilizing advanced mathematics for the benefit of precision medicine,” says Schreiner.
Use in Clinical Practice
“The overall aim of the comprehensive cancer center of the Medical University of Vienna and Vienna General Hospital is to treat patients more selectively and individually,” says Heinz Kölbl, MD, Drhc, head of the hospital’s division of general gynecology and gynecologic oncology, which also participated in the study.“The challenge is to offer tailor-made therapy so that we can give the correct treatment in a more targeted and accurate way, thereby avoiding the use of unnecessary treatments and associated side-effects.”
“Since receptor status continues to be one of the most important parameters in terms of tumor biology, adding molecular biological data to traditional immunohistochemistry is a step towards more-precise tumor characterization,” says Christian Singer, MD, member of the comprehensive cancer center, head of senology, and head of the laboratory for hereditary breast and ovarian cancer in the university’s department of obstetrics and gynecology. “If the results are confirmed in independent studies, this will be an important qualitative step, providing doctors and patients with an unprecedented degree of diagnostic certainty.”
Reference
- Kenn M, Cacsire Castillo-Tong D, Singer CF, Cibena M, Kölbl H, Schreiner W. Co-expressed genes enhance precision of receptor status identification in breast cancer patients. Breast Cancer Res Treat. 2018;172(2):313–326; doi: 10.1007/s10549-018-4920-x.
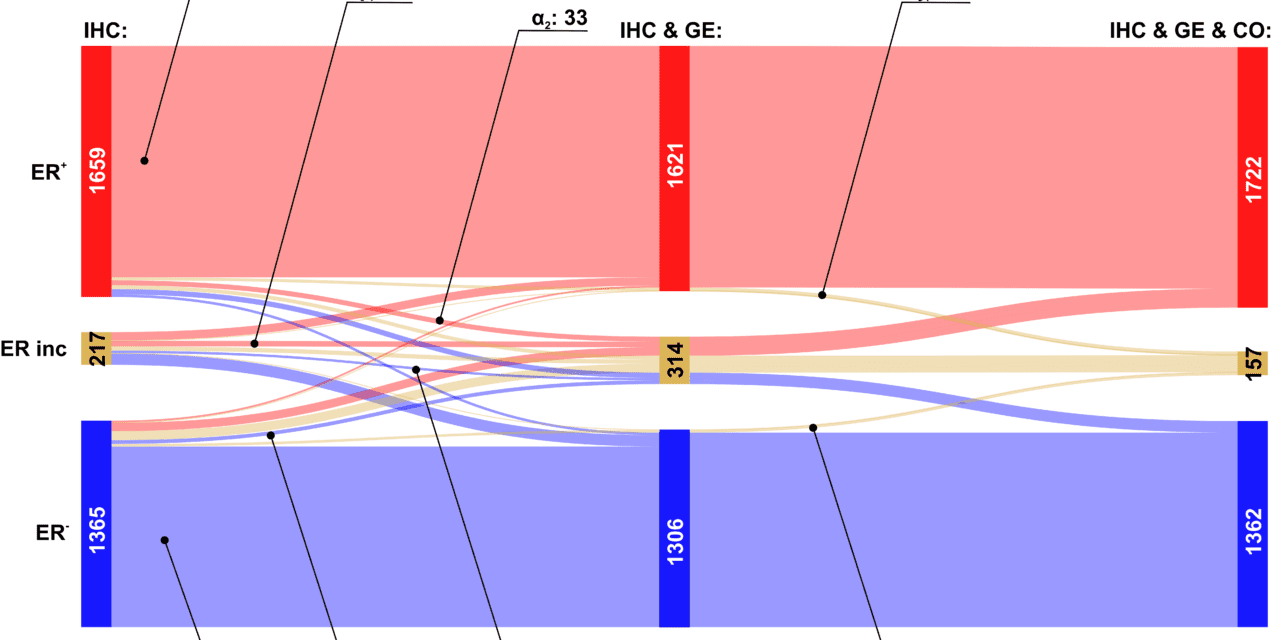
Featured image: More information, more safety for breast cancer patients. Selecting optimum therapy for each individual requires hormone receptors be precisely determined. Starting with basic IHC data (left), and supplementing it with genome data (middle, right) adds confidence to the result.