Taking a systems approach assures quality care for critically ill patients
By Shara Rosen
Since its introduction in the 1950s, the analysis of arterial blood gases—as indicated by measurements of acidity (pH), partial pressures of oxygen (PO2), and carbon dioxide (PCO2)—has been central to management of the most critically ill patients in a hospital. Continued technology enhancements and innovations in blood gas instrumentation have reduced test times to less than a minute and decreased the amount of blood needed from milliliters to microliters. Information technologies have also advanced the field, providing algorithms that have expanded the sample type to include capillary blood samples that can be used when an arterial sample may be difficult to get.
 Over the past few years, two trends have further spurred the evolution of blood gas testing. CLP has consulted with industry professionals to get a sense of some of the issues resulting from these trends and how vendors and caregivers are addressing those issues. Among the experts interviewed for this article, the consensus is that an increasing amount of routine testing is being moved out of laboratories, and is winding up closer and closer to the patient’s bedside.
Over the past few years, two trends have further spurred the evolution of blood gas testing. CLP has consulted with industry professionals to get a sense of some of the issues resulting from these trends and how vendors and caregivers are addressing those issues. Among the experts interviewed for this article, the consensus is that an increasing amount of routine testing is being moved out of laboratories, and is winding up closer and closer to the patient’s bedside.
“We are seeing a trend to moving more and more routine testing to the bedside,” says Bruce Lewis, marketing manager for the Epoc blood analysis system by Alere Inc, San Diego. “This has created more demand for portable multianalyte test devices that can provide quick results at the bedside for critically ill patients, and at care sites where immediate results are important.”
According to Brad Bullen, product manager for Nova Biomedical, Waltham, Mass, it is not necessarily important to use a portable device, but any instrument that offers many analytes and has multiple applications is attractive because all the tests are on one platform. Nova Biomedical’s Stat Profile pHOx Ultra, for example, offers testing for more than 21 analytes.
Together with the three basic analytes, such blood gas menu expansion may include electrolytes, glucose, ionized calcium, ionized magnesium, blood urea nitrogen, creatinine, lactate, hemoglobin fractions, bilirubin, and other analytes. Most of these are available on current analyzers. The test menu on the i-STAT system from Abbott Point of Care, Princeton, NJ, also includes cardiac markers (BNP, CK-MB, and Troponin I) and coagulation testing (ACT and PT/INR).
Thus, from a single whole-blood sample, in a minute or less, blood gas analyzers can produce a very clear picture of the patient’s acid/base, respiratory, cardiovascular, and metabolic status.
There is also a consensus that critical care analytes are best run as soon as possible after the blood has been drawn. Thus, more and more instruments are found throughout the hospital, nearer the patient.
THE WHOLE PICTURE: A SYSTEMS APPROACH
“The goal is an end-to-end strategy, a point-of-care (POC) ecosystem that provides scalable, correlated, quality solutions that match the customers’ needs in the setting where it is needed,” explains David Stein, CEO of the POC business unit at Siemens Healthcare Diagnostics, Tarrytown, NY. “This ecosystem assures that a POC coordinator can control and monitor instruments spread throughout the healthcare system as if they were in a virtual room.”
Such a systems approach is critical to quality results and patient care, agrees Alan Beder, senior product manager at Radiometer America Inc, Westlake, Ohio. “You can have the best instrument, but it is the whole testing process and what goes into providing the blood gas service that contributes to quality patient care.”
PREANALYTICAL STEPS ARE CRITICAL
It all starts with the preanalytical phase, says Beder. “We tend to focus on the analyzer, but really, you have to look at collecting the sample correctly, removing air bubbles, and mixing correctly, so as to avoid clots and assure a homogenous sample.”
One of the top issues is preventing preanalytical errors, mainly because menus have grown. “Often, caregivers are not aware of which heparin to use and how to properly manage the sampling process—such as filling the syringe correctly,” says John Ancy, clinical specialist at Instrumentation Laboratory, Bedford, Mass. “This is a very simple operation where errors can be rectified with proper training.”
In addition, Ancy explains, microsensors have replaced macroelectrodes, so the pathways are smaller, making it even more important to mix the sample very well and immediately after it has been drawn to prevent microclots. Not all operators have been sensitized to how important this is.
Vendors have designed samplers that help mitigate sampling and mixing issues.1 Radiometer markets the SafePico syringe that includes a device to remove air bubbles, and also has a ball in the syringe that mixes the sample. The company also provides an automated mixer that can be used at the bedside.
Instrumentation Laboratory’s GEM EasyDraw and GEM SafetyDraw aspirators and syringes have been developed to optimize sample quality and results. Similarly, Siemens’ RapidLyte arterial blood gas sampling syringes and Multicap capillaries are designed to help minimize preanalytical error. Nova Biomedical has developed a clot-block technology that prevents a clot from entering into the sample line.

The Opti R blood gas analyzer by Opti Medical Systems has an auto-aspiration feature that makes sure the test cartridge is filled properly and also includes bubble and clot detection.
The Opti R analyzer uses the company’s proprietary Opti Quality Monitor software to ensure accurate results from each measurement, explains Britteny Garner, marketing manager for Opti Medical Systems, Roswell, Ga. The Opti has an auto-aspiration feature that makes sure the test cartridge is filled properly and also includes bubble and clot detection. Another feature is a check for cartridge packaging integrity and proper storage.
IQCP: PROCESS CONTROL
For nonwaived tests, the Individual Quality Control Plan (IQCP) program of the Centers for Medicare & Medicaid Services is a major driver for improving every phase of the blood gas preanalytical process—and especially operator competency. “IQCP has been a long time overdue,” says Bullen. “For patient safety, it is really crucial to make sure that a device is functional at all times.”
[reference id=”39930″]Sidebar: Specimen Collection and Patient’s Body Temperature[/reference]
Companies have already undertaken a number of initiatives to support the IQCP program. The IQCP education and transition period began on January 1, 2014, and will conclude when the program goes fully into effect on January 1, 2016.
The IQCP program is expected to address one of the biggest preanalytical challenges in operator training and competency. All of the blood gas instrument vendors provide guides that include training information and also explain basic blood gas parameters and underlying metabolic conditions.
Garner explains that in some of the emerging markets where Opti systems are used, the company had to provide a very basic educational component, because “sometimes users did not understand why they should run a blood gas or how to interpret the test results.”
DATA MANAGEMENT
“One of the things we look at is downstream interfacing in terms of both getting orders into an instrument and getting data to the clinician,” says Geoffrey Baird, MD, PhD, assistant professor of laboratory medicine at the University of Washington. “This is a very important consideration, and while it is generally available on today’s instruments, we look at the quality and ease of use of the interface and the cost.”
“Beyond the preanalytical phase, we are seeing a focus on data accuracy,” says Radiometer’s Beder. “The Joint Commission has adopted National Patient Safety Goals that include the use of two patient identifiers, so one of the things we have implemented is integrating the syringe with the information system.” In this way, he explains, the patient information and test information are both automatically transferred to the lab and hospital IT systems, and they can also be reviewed at the bedside where they were initially registered.
Alere’s Epoc system also incorporates advanced IT features to protect patient safety and ensure proper handling of test data. “To ensure that the right test is done on the right patient, the test card is read by the Epoc system’s integrated personal digital assistant, which operates similar to a smart phone,” says Alere’s Lewis. “The system also transmits patient and test data directly to the provider’s electronic medical record or laboratory information system. Thus, data are automatically transmitted to the site of care as well as to members of the care team, no matter where they may be located.”
A Siemens instrument user can use a smart phone or a tablet to remotely access the RapidComm system that forms the backbone of the company’s laboratory ecosystem, says Stein. Using this system, he adds, “a POC coordinator can manage the instrument remotely—and basically do everything but add the sample.”
Essentially, all of the vendors that offer blood gas analyzers also offer some form of data communication solution. However, data communication is still a challenge, says Ancy. “Beyond the quality of the data, there are network problems, server problems, interruptions, and interface issues. I think we are still in a development phase of data communication and electronic management of medical records.
“Wi-Fi communication is still developing, and is definitely going to be universal in medical devices in the not-too-distant future,” adds Ancy. At this time, only Alere’s Epoc and Radiometer’s ABL90 Flex blood gas analyzers offer wireless communication.
COST IS ANOTHER FACTOR
“One thing that is always on the mind of lab professionals is cost,” says Baird. “Because the menus are all essentially the same, the operating principles are basically the same, and all instruments offer a fast test turnaround time—so, honestly, we look at cost. We look at how a device is presented, the acquisition options that are offered, and how much it will cost,” he adds.
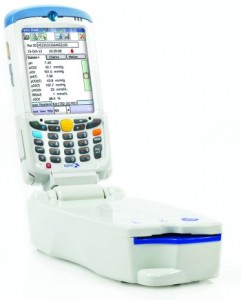
The Epoc blood analysis system by Alere incorporates advanced IT features to protect patient safety and ensure proper handling of test data.
There is a trade-off between maintenance and cost, says Baird. Some instruments are more expensive per test because the maintenance is contained in the cartridge, and they are otherwise almost maintenance free. For other instruments, however, reagents may be less expensive, but they require more extensive maintenance procedures. “That is a calculation that lab directors have to take into consideration,” he says. “What do we want to spend our time doing, and what makes sense economically for each lab and hospital?”
Alere has addressed some of the issues related to the cost of cartridge-based testing. Each single-use Epoc BGEM test card contains a menu of 11 analytes and can be stored at room temperature for 6 months. This helps with inventory management, explains Lewis.
THE BOTTOM LINE
Near-patient blood gas testing anywhere in the world has evolved to a more systems approach where sample quality, operator competency, and data transfer are of primary concern. An important focus is to have minimal maintenance and an easy-to-use interface, so that a quality test result can be produced and communicated to the caregiver quickly.
First and foremost, vendors and operators focus on all the preanalytical steps that might jeopardize sample quality and thus produce a test result that does not really reflect the actual status of the patient. Blood gases are run on the very sickest of patients; caregivers must be able to act on those results with confidence.
REFERENCES
1. Grenache DG, Parker C. Integrated and automatic mixing of whole blood: an evaluation of a novel blood gas analyzer. Chimica Acta. 2007;375(1–2):153–157.
2. National Patient Safety Goals. Two Patient Identifiers: NPSG 1 01.01.01. December 9, 2008. Available at: www.jointcommission.org/mobile/standards_information/jcfaqdetails.aspx?StandardsFAQId=145&StandardsFAQChapterId=77. Accessed October 13, 2014.
Shara Rosen is a contributing writer for CLP. For more information, contact CLP chief editor Steve Halasey via [email protected].