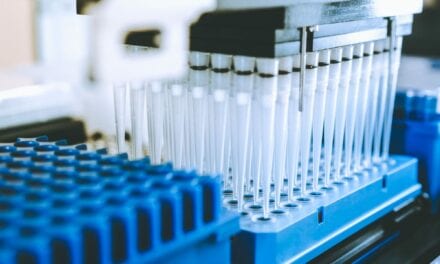
Protecting sample stability ensures the utility of the latest generation of TB tests
By William Cruikshank, PhD
Tuberculosis (TB) infection and disease continues to be a global health crisis. In the United States, more than 11 million people are infected with TB, and without treatment 5% to 10% will progress to active disease. Essential for controlling TB disease is identifying infected patients. However, the most commonly used test to confirm TB infection, the tuberculin skin test (TST), presents challenges with both compliance and confounding results.
Blood tests called interferon-gamma release assays (IGRAs) have recently been shown to offer improved accuracy, convenience, and compliance for TB testing. With the increased time required to conduct IGRAs, however, some questions have been raised about blood sample stability related to the use of stabilizing agents in IGRAs.
Review of available data indicates that use of an FDA-approved blood stabilizer in IGRA TB testing provides a range of potential advantages to public health and laboratory professionals, including expanded time required for sample storage and transport. Clinical studies demonstrate that use of stabilizers in IGRA testing does not negatively affect testing sensitivity.
This article will explore recent findings regarding the use of IGRA blood-based TB testing, including considerations related to blood sample stability and the use of stabilizing agents to support extended storage and transportation times for blood samples.
Global Burden, Global Goals
In 2014 the global burden for individuals manifesting TB infection was estimated to be 23% (1.7 billion people), with 9.6 million people progressing to active TB disease, and approximately 1.5 million deaths resulting from the disease.1,2 It is estimated that someone infected with TB has a 5% to 10% probability of progressing to active disease during their lifetime.3
Thus far, the mechanisms involved in the transition process are not well understood. However, factors that affect the immune system appear to be contributory, as a number of risk factors for progression have been identified, including alcohol use, HIV, smoking, type 2 diabetes, young age, and the use of immunosuppressants for autoimmune diseases.4–9 Without treatment, an infectious individual is likely to transmit infection to 3–10 people annually, indicating a relatively low rate of transmission. Nevertheless, the disease remains highly lethal, as approximately 50% of those who remain untreated will die from the disease.10 During the past couple of years, TB has surpassed HIV/AIDS as the leading cause of death for any single pathogen.11
In May 2014, the World Health Assembly adopted a “global strategy and targets for tuberculosis prevention, care, and control after 2015”—an initiative put forth by the World Health Organization (WHO).12 WHO’s “End TB Strategy” has set the goals of a 95% reduction in the number of TB deaths, and a 90% reduction in the TB incidence rate, by the year 2035.13 To best achieve these goals, there must be an understanding of the worldwide reservoir of TB infection as well as the capacity to accurately identify and distinguish those who have been infected with TB from those who have active TB disease.
Detecting TB Infection
In 1910, French physician Charles Mantoux presented data supporting the concept that individuals infected with TB could be identified by the presence of an induration following intradermal injection of a purified protein derivative (PPD) from TB. Turned into a test, termed the tuberculin skin test (TST), Mantoux’s concept relied on his observation that the presence of TB proteins in a TB-infected individual will initiate a delayed hypersensitivity reaction within 48–72 hours. A number of factors must be considered to accurately interpret the TST, including the individual’s overall health and pre-test probability of infection as well as the precise measurement of the induration.14
Advantages of TST are that it is an in vivo test that requires few reagents and no sample manipulation, can be conducted by a healthcare provider with minimal training, and is perceived to be cost-effective. For these reasons, TST is frequently used in resource-poor settings. Limitations of TST include crossreactivity with bacillus Calmette–Guérin, used for vaccines, as well as crossreactivity in individuals infected with nontuberculous mycobacteria.15,16 In addition to crossreactivity, the test is also limited by the subject’s compliance with respect to completing a second visit to assess induration 48–72 hours following TST placement.

Figure 1. Close-up of blood specimens for the T-Spot TB test before being processed by technicians at Oxford Diagnostic Laboratories.
These issues associated with TST have reduced the global utility of the test and highlighted the need for a test with less crossreactivity and higher compliance potential. In response to this need, two in vitro tests have been developed to assess the immune response to stimulation by select TB antigens. For both tests, the underlying concept is to quantify interferon-gamma (IFN?) production by TB-sensitized T-effector lymphocytes following stimulation with antigenic TB proteins, which are not produced by either bacillus Calmette–Guérin or by most nontuberculous mycobacteria strains, and therefore eliminate the potential for crossreactivity.
The two tests differ in their methods for detecting generation of IFN???The T-Spot TB test uses an enzyme-linked immunospot (ELISPOT) platform from Oxford Immunotec, Abingdon, UK, while the QuantiFeron Gold In-Tube test uses the QFT ELISA platform from Qiagen, Germantown, Md. Unlike TST, for which the induration results from T-effector and T-memory cell activation following intradermal placement of >200 TB antigens, the two interferon-gamma release assays (IGRAs) assess in vitro responsiveness of a select subset of cells—T-effector cells—when stimulated by a limited number (2–3) of TB antigens.17 Using such a targeted approach has in most reports identified IGRAs as having increased sensitivity, specificity, and a reported increase in patient compliance as compared with TST.18
Comparing IGRA Platforms
Although IFN? is the common analyte for both IGRAs, the two tests use completely different platforms to quantify production of the cytokine. The ELISA platform uses whole blood collected in three different tubes that contain either TB antigens (CFP10, ESAT-6, and TB 7.7), PHA as a positive control, or no antigen as a negative control. Following phlebotomy, the tubes are shaken to expose the cells to the antigens and then incubated at 37°C for 16–20 hours, at which time the plasma is isolated and IFN? production assessed by standard ELISA technique.19 This process results in stimulation of the TB-sensitized cells contained in the 1cc of whole blood collected in each tube.
The ELISPOT platform takes a different approach, using isolated peripheral blood mononuclear cells (PBMCs), which are washed and then resuspended in culture media to a normalized number of 250,000± cells per well (see Figures 1, 2). This approach allows for a standardized number of PBMCs in each well, independent of clinical conditions such as leukopenia, which can alter endogenous PBMC numbers. Following isolation, cells are divided among four wells containing CFP10, ESAT-6, PHA (positive control), and media alone (negative control) on a 96-well plate, and incubated for 16–20 hours. IFN? produced by antigen-sensitized cells is captured by plate-bound anti-IFN? antibody and, following a substrate reaction, the number of spots in each well is then quantified.20
In general, the two different methodological platforms provide different efficiencies when assessing test results for individuals with confirmed active TB. The ELISA method quantifies total detectable IFN? present in the plasma following antigenic stimulation, while the ELISPOT method quantifies the number of antigen-sensitized cells that produce IFN? following antigen stimulation.
According to guidelines issued by the US Preventive Services Task Force, the ELISA platform (QuantiFeron Gold In-Tube) provides sensitivity of 80% (24 studies/2321 subjects), and specificity of 97% (4 studies/2053 subjects).21 By contrast, the ELISPOT platform (T-Spot TB test) achieved sensitivity of 90% (16 studies/984 subjects), and specificity of 95% (5 studies/1810 subjects). The T-Spot TB test results are qualitative and are reported as positive, borderline, or negative, provided that the test controls perform as expected. Test results are determined by enumerating the IFNg spots from individual T cells captured in each of the patient’s four test wells (positive control, negative control, panel A, panel B).
Increasing T Lymphocyte Stability
The manner in which blood samples are handled prior to conducting a specific test is important for all in vitro assays. If such preanalytic steps are not conducted in a consistent, reproducible fashion, the test results can be affected. This concept is particularly important when time to processing following venipuncture is hours long, thereby allowing for changes to occur to the cells, now in a different environment.
As an example, studies have indicated that the presence of granulocytes (primarily neutrophils) 8 hours following venipuncture can affect the responsiveness of T lymphocytes to antigenic stimulation.22 This effect can be attributed, at least in part, to the generation of hydrogen peroxide by the neutrophil, which reduces the ability of the T lymphocyte to produce cytokines such as IFN?.23
To avoid problems resulting from prolonged blood storage prior to conducting the test, both IGRAs have incorporated steps that help to maintain T lymphocyte responsiveness. The QuantiFeron test adopted the strategy of drying the antigens onto the sides of the sample tubes rather than suspending them in a liquid.19 This approach prolonged storage time to 16 hours before the blood had to be processed.

Figure 3. Above, technicians at Oxford Diagnostic Laboratories processing T-Spot TB test specimens using standard laboratory techniques and equipment.
For the T-Spot TB test, Oxford Immunotec developed a different approach. The T-Spot TB test is available as a kit that can be performed in a local laboratory. In the United States, however, most T-Spot TB tests are performed by Oxford Diagnostic Laboratories at the company’s centralized laboratory in Memphis, Tenn. Most blood samples must therefore be shipped to the lab overnight, increasing the time required to maintain T-lymphocyte responsiveness (see Figure 3).
To meet the need for extended blood storage, Oxford Immunotec developed a step designed to significantly reduce granulocyte contamination and maintain T lymphocyte responsiveness and appropriate cytokine production.20,24 Such prolonged storage of whole blood can result in granulocyte activation, degranulation, and subsequent secretion of cytokines and superoxide anions.23 In turn, the loss of these factors reduces cellular density, resulting in less-effective removal from PBMCs following density centrifugation.25
Granulocyte contamination during PBMC preparation creates two problems. The first problem is that the standardized number of PBMCs plated in each well (250,000± cells) can now include contaminating granulocytes, which would dilute the number of targeted antigen-specific T lymphocytes and potentially reduce the sensitivity of the test. The second problem is that the presence of granulocytes, which are still likely producing hydrogen peroxide, can interfere with lymphocyte production of IFN?, also possibly reducing test sensitivity.23
To effectively reduce granulocyte contamination, Oxford Immunotec incorporated a step just prior to density centrifugation, increasing the density of the granulocytes so that they will pass through the density medium during centrifugation.20 To accomplish this, the Oxford Immunotec method adds to the blood sample a reagent called T-Cell Xtend, an antibody complex that binds to both red blood cells (RBCs) and CD66b, a protein expressed on activated granulocytes.26 The antibody acts to bridge the two cell types, creating a cell-cell complex with increased density during gradient centrifugation. The result is similar to what is achieved when processing freshly isolated blood: a highly enriched PBMC preparation with typically less than 2% contaminating granulocytes.27
A number of clinical studies have reported very high congruency between T-Spot TB test results using T lymphocytes from freshly isolated blood and from blood stored up to 32 hours prior to isolation. Such study results demonstrate that granulocyte depletion using the T-Cell Xtend reagent is sufficient to maintain T lymphocyte responsiveness to TB antigen stimulation.28–30 As an example, one study tested more than 300 paired samples taken at a wide array of times.30 The study demonstrated an overall agreement for the paired tests at 95.4% (288/302; range 92.3–97.4%). An important component of this study was that it included subjects who had increased risk factors for TB (asthma, diabetes, HIV coinfection, and steroid treatment), demonstrating that even in samples from immunocompromised individuals, the T-Cell Xtend reagent maintains T-cell responsiveness without negatively affecting test results.30 The T-Cell Xtend reagent received FDA approval for use with the T-Spot TB test in 2010.
Maintaining Test Sensitivity
Although a number of studies have reported test sensitivity greater than 93% with the use of the T-Cell Xtend reagent, two studies in particular are of interest as they also include immunocompromised subjects. One study conducted in Tanzania involved 66 TB culture-confirmed subjects, 26% of whom were also HIV-1 positive.28 For samples that used the T-Cell Xtend reagent, the investigators reported a 95.4% agreement between the T-Spot TB test results and culture results that calculated to an overall sensitivity of 96.8%.
The second study looked at a different immunocompromised population: the elderly.31 The elderly are more susceptible to TB infection due to a decline in the immune response associated with age, which also renders detection of TB infection based on immune responses far more difficult.31 This study investigated the sensitivity of the T-Spot TB test, using the T-Cell Xtend reagent, in different age groups, including individuals aged 70 and above.32 The study enrolled 212 subjects in different age groups and reported that for subjects aged less than 50 the average sensitivity was 95.7%; for subjects aged between 50 and 69, there was a slight decrease in sensitivity to 87.5%; and in subjects aged 70 and above, sensitivity was maintained at 85.7%. This study demonstrated the high sensitivity and reliability of the T-Spot TB test even among older age groups, for which detection can be extremely challenging.
Conclusion
To successfully implement and complete WHO’s “End TB Initiative,” a screening strategy must exist that can identify the 23% of the world’s population infected with TB—and especially those who are classified as high-risk individuals. IGRAs have proven to be more sensitive and reliable than TST, particularly where bacillus Calmette–Guérin vaccines are common; but they require time associated with blood transportation and processing, thereby increasing the risk of reduced T-lymphocyte responsiveness.
Use of the T-Cell Xtend reagent to maintain T-lymphocyte responsiveness provides flexibility for instances when blood samples cannot be processed within 8 hours of venipuncture. Such flexibility is particularly important not only for healthcare sites that use overnight shipping to the central laboratory for sample processing, as in the United States, but for remote sites around the world that do not have access to a local laboratory and require shipping for sample processing. Having a processing window of 32 hours allows for longer distances between the draw site and the processing site, and also enables labs to accommodate potential delays in sample transportation.
Existing clinical data provides confidence that samples shipped to distant labs will not be negatively affected. While additional screening tools are required to better predict which infected individuals will progress to active TB disease, the expanded use of existing screening tests, such as IGRAs, should provide valuable information to help identify the world’s TB reservoir.
William Cruikshank, PhD, is director of scientific affairs at Oxford Immunotec, Abingdon, UK. For further information, contact CLP chief editor Steve Halasey via [email protected].
References
- Houben RM, Dodd PJ. The global burden of latent tuberculosis infection: a reestimation using mathematical modeling. PLoS Med. 2016;13(10):e1002152; doi: 10.1371/journal.pmed.1002152.
- Global Tuberculosis Report 2015. 20th ed. Geneva: World Health Organization; 2015.
- Vynnycky E, Fine PE. The natural history of tuberculosis: the implications of age-dependent risks of disease and the role of reinfection. Epidemiol Infect. 1997;119(2):183–201.
- Havlir DV, Getahun H, Sanne I, Nunn P. Opportunities and challenges for HIV care in overlapping HIV and TB epidemics. JAMA. 2008;300(4):423–430; doi: 10.1001/jama.300.4.23.
- Jeon CY, Murray MB. Diabetes mellitus increases the risk of active tuberculosis: a systematic review of 13 observational studies. PLoS Med. 2008;5(57):e152; doi: 10.1371/journal.pmed.0050152.
- Dodd PJ, Sismanidis C, Seddon JA. Global burden of drug-resistant tuberculosis in children: a mathematical modeling study. Lancet Infect Dis. 2016;16(10):1193–1201; doi: 10.1016/S1473-3099(16)30132-3.
- Rehm J, Samokhvalov AV, Neuman MG, et al. The association between alcohol use, alcohol use disorders and tuberculosis (TB): a systematic review. BMC Public Health. 2009;9:450; doi: 10.1186/1471-2458-9-450.
- Bates MN, Khalakdina A, Pai M, Chang L, Lessa F, Smith KR. Risk of tuberculosis from exposure to tobacco smoke: a systematic review and meta-analysis. Arch Intern Med. 2007;167(4):335–342.
- Singanayagam A, Manalan K, Sridhar S, et al. Evaluation of screening methods for identification of patients with chronic rheumatological disease requiring tuberculosis chemoprophylaxis prior to commencement of TNF-alpha antagonist therapy. Thorax. 2013;68(10):955–961; doi: 10.1136/thoraxjnl-2013-203436.
- Andrews JR, Noubary F, Walensky RP, Cerda R, Losina E, Horsburgh CR. Risk of progression to active tuberculosis following reinfection with Mycobacterium tuberculosis. Clin Infect Dis. 2012;54(6):784–791; doi: 10.1093/cid/cir951.
- Sulis G, Centis R, Sotgiu G, et al. Recent developments in the diagnosis and management of tuberculosis. NPJ Prim Care Respir Med. 2016;26:16078; doi: 10.1038/npjpcrm.2016.78.
- Uplekar M, Weil D, Lonnroth K, et al. WHO’s new end TB strategy. Lancet. 2015;385(9979):1799–1801; doi: 10.1016/S0140-6736(15)60570-0.
- The End TB Strategy: Global Strategy and Targets for Tuberculosis Prevention, Care, and Control after 2015. Geneva: World Health Organization, 2014. Available at: www.who.int/tb/strategy/End_TB_Strategy.pdf?ua=1. Accessed March 23, 2017.
- Farhat M, Greenaway C, Pai M, Menzies D. False-positive tuberculin skin tests: what is the absolute effect of BCG and non-tuberculous mycobacteria? Int J Tuberc Lung Dis. 2006;10(11):1192–1204.
- Menzies D, Gardiner G, Farhat M, Greenaway C, Pai M. Thinking in three dimensions: a web-based algorithm to aid the interpretation of tuberculin skin test results. Int J Tuberc Lung Dis. 2008;12(5):498–505.
- Pai M, Riley LW, Colford JM Jr. Interferon-gamma assays in the immunodiagnosis of tuberculosis: a systematic review. Lancet Infect Dis. 2004;4(12):761–776.
- Mack U, Migliori GB, Sester M, et al. LTBI: latent tuberculosis infection or lasting immune responses to M. tuberculosis? a TBNET consensus statement. Eur Respir J. 2009;33(5):956–973.
- Wrighton-Smith P, Sneed L, Humphrey F, Tao X, Bernacki E. Screening health care workers with interferon-gamma release assay versus tuberculin skin test: impact on costs and adherence to testing (the SWITCH study). J Occup Environ Med. 2012;54(7):806–815.
- QuantiFeron-TB Gold (QFT) ELISA [package insert]. Germantown, Md: Qiagen; 2013.
- T-Cell Xtend [package insert PI-TT.610-US-V5]. Abingdon, UK: Oxford Immunotec Ltd; 2014.
- Bibbins-Domingo K, Grossman DC, Curry SJ, et al. Screening for latent tuberculosis infection in adults: US Preventive Services Task Force recommendation statement. JAMA. 2016;316(9):962–969; doi: 10.1001/jama.2016.11046.
- Bull M, Lee D, Stucky J, et al. Defining blood processing parameters for optimal detection of cryopreserved antigen-specific responses for HIV vaccine trials. J Immunol Methods. 2007;322(1–2):57–69.
- Schmielau J, Finn OJ. Activated granulocytes and granulocyte-derived hydrogen peroxide are the underlying mechanism of suppression of T-cell function in advanced cancer patients. Cancer Res. 2001;61(12):4756–4760.
- McKenna KC, Beatty KM, Vicetti MR, Bilonick RA. Delayed processing of blood increases the frequency of activated CD11b+ CD15+ granulocytes which inhibit T-cell function. J Immunol Methods. 2009;341(1–2):68–75; doi: 10.1016/j.jim.2008.10.019.
- Lewis SL, Van Epps DE, Chenoweth DE. Analysis of density changes and chemotactic receptors of leukocytes from chronic hemodialysis and peritoneal dialysis patients. Blood Purif. 1987;5(2–3):138–154.
- Futosi K, Fodor S, Mócsai A. Neutrophil cell surface receptors and their intracellular signal transduction pathways. Int Immunopharmacol. 2013;17(3):638–650; doi: 10.1016/j.intimp.2013.06.034.
- Fuss IJ, Kanof ME, Smith PD, Zola H. Isolation of whole mononuclear cells from peripheral blood and cord blood. Curr Protoc Immunol. 2009;Chapter 7:Unit7.1; doi: 10.1002/0471142735.im0701s85.
- Talbot EA, Maro I, Ferguson K, et al. Maintenance of sensitivity of the T-Spot TB assay after overnight storage of blood samples. Dar es Salaam, Tanzania. Tuberc Res Treat. 2012;2012:345290; doi: 10.1155/2012/345290.
- Higuchi K, Sekiya Y, Igari H, Watanabe A, Harada N. Comparison of specificities between two interferon-gamma release assays in Japan. Int J Tuberc Lung Dis. 2012;16(9):1190–1192; doi: 10.1155/2012/345290.
- Wang SH, Stew SS, Cyktor J, Carruthers B, Turner J, Restrepo BI. Validation of increased blood storage times with the T-Spot TB assay with T-Cell Xtend reagent in individuals with different tuberculosis risk factors. J Clin Microbiol. 2012;50(7):2469–2471; doi: 10.1128/JCM.00674-12.
- Rajagopalan S. Tuberculosis in older adults. Clin Geriatr Med. 2016;32(3):479–491; doi: 10.1016/j.cger.2016.02.006.
- Bae W, Park KU, Song EY, et al. Comparison of the sensitivity of QuantiFeron-TB Gold In-Tube and T-Spot TB according to patient age. PLoS One. 2016;11(6):e0156917; doi: 10.1371/journal.pone.0156917.