By Michael A. Pfaller, MD, and Thomas J. Lowery, PhD
In patients who suffer from invasive septic infections such as invasive candidiasis, the titer levels of pathogens are typically less than 10 colony-forming units (CFU)/mL, and can even be below 1 CFU/mL. Today’s gold standard for detection of invasive candidiasis is blood culture, despite having a clinical sensitivity of only 60%.
In recent years, several tests utilizing technologies ranging from mass spectrometry to polymerase chain reaction (PCR) have been introduced to aid in the diagnosis of invasive candidiasis. However, the extremely low titer levels of invasive candidiasis are undetectable by these competing testing methods—even those utilizing PCR. All other methods cleared by FDA for the detection of Candida pathogens in blood samples are performed on samples from positive blood cultures. Other methods that have been CE marked for use in Europe have limits of detection of 30 CFU/mL or higher.

Figure 1. The T2Dx instrument is a random-access, moderate-throughput analyzer that can process up to seven samples in parallel.
An alternative to such technologies based on magnetic resonance has recently been introduced to the clinical microbiology testing market by T2 Biosystems, Lexington, Mass (see Figure 1). Introduction of the T2Candida panel and T2Dx instrument represents a new class of highly sensitive tests for measurement of invasive bloodstream infections directly from a blood draw. The T2Candida panel and T2Dx instrument are both FDA cleared and CE marked, and are commercially available in the United States and Europe. The T2Dx instrument is fully automated from sample to answer, and is designed to run as a moderate-complexity test in a hospital laboratory certified under the terms of the Clinical Laboratory Improvement Amendments of 1988 (CLIA).
The distinguishing characteristics of the T2Candida panel and T2Dx instrument are that they enable unprecedented analytical and clinical sensitivity for invasive bloodstream infections and have been demonstrated to have much higher clinical sensitivity (91.1%) than the existing gold standard blood culture (60%).
This article provides an overview of the diagnostic and therapeutic challenges associated with invasive candidiasis, describes how the T2MR technology works, summarizes some of the key performance data developed in studies of the technology, and discusses how implementation of the T2Candida panel can improve patient outcomes.
Current Diagnostic Approaches to Invasive Candidiasis
Invasive candidiasis is the most important fungal infection detected among hospitalized individuals worldwide.1 In European and North American intensive care units, Candida has been found to be the second most common infection, after Staphylococcus aureus (see Figure 2). And in the United States, Candida is presently the third leading cause of catheter-related bloodstream infections.2
It is widely recognized that early diagnosis of candidiasis is difficult.3 The clinical signs and symptoms of candidiasis are nonspecific and often appear late in the course of infection. Because of the critically ill nature of most high-risk patients, invasive diagnostic procedures may be considered too risky. And the entire diagnostic process is negatively affected by the lack of sensitive and minimally invasive assays.

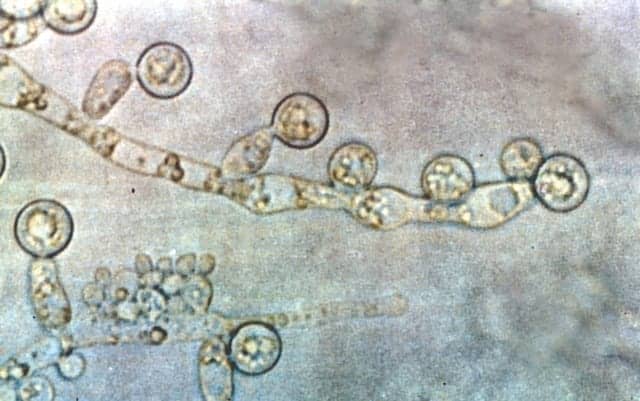
Figure 2. The T2Candida panel detects the five clinically relevant species of Candida, including C. albicans, which is a common fungal sepsis-causing pathogen.
Given the recognized prominence of Candida as a cause of healthcare-associated infection, it is now appreciated that delays in initiating appropriate antifungal therapy are associated with significant increases in both patient mortality and the cost of care for patients with candidemia.3 It has been estimated that each day of delay before initiating antifungal therapy is associated with a 50% increase in patient mortality and an additional $5,000 in healthcare costs.
A seminal study about the effects of delayed initiation of treatment for candidemia found that delays of 12 to 24 hours were independent determinants of in-hospital mortality. While initiation of treatment without delay was associated with a mortality rate of 11.1%, delays greater than 12 hours resulted in a mortality rate of 33.1%.4
Because Candida infection generally occurs among patients with a large number of comorbidities, it is associated with greater mortality (49%) and longer periods of hospitalization (30 days) than most other healthcare-associated infections (HAIs).1 Likewise, the costs associated with Candida infection are among the highest associated with any HAI, ranging from $6,214 to $142,394 per patient.
Nevertheless, the majority of patients with invasive candidiasis do not receive antifungal therapy until the time of yeast detection in culture, and many patients are not placed on the appropriate therapy until the Candida species is identified.
Most institutions that care for high-risk patients offer comprehensive microbiology services that include both species-level identification as well as antifungal susceptibility testing of Candida species from blood and other normally sterile sites. But improving the diagnosis and management of Candida infections will require a much more rapid, sensitive, and specific approach to diagnosis as well as increased attention to the time-sensitive aspects of administering antifungal therapy.3
Blood Culture. Despite the fact that blood culture has always been considered too slow and insensitive to serve as an early diagnostic method, the use of blood culture remains an established approach to the diagnosis of candidiasis, and is at the heart of care guidelines for candidiasis among hospitalized individuals.5,6
Because contemporary blood culture methods demonstrate variable sensitivity—especially at low concentrations of Candida in the blood sample—current practice is to serially collect multiple aerobic and anaerobic blood culture specimens over 24 to 48 hours. Positive blood cultures must be subjected to Gram stain and post-culture identification, processes that require additional time and technical expertise.
Yet it is increasingly apparent that as many as one-third of patients with invasive candidiasis never produce a positive blood culture. In one review performed on 415 autopsy-proven cases of candidiasis, researchers found that blood cultures were positive in only 38% of cases.7 And such a low yield for blood culture was confirmed in a meta-analysis of 10 studies for the diagnosis of invasive candidiasis, where the researchers reported a similar pooled blood culture positivity rate of 38%.8
Cultures of blood and other clinical specimens may also be rendered falsely negative by the use of prophylactic or empiric antifungal therapy, further confounding efforts to establish a firm diagnosis. And even when a culture is deemed positive, species-level results may not be available for 48 to 72 hours—or longer.
As it is now understood that gathering the information required to limit mortality and the emergence of antifungal resistance is a time-critical procedure, it should be equally clear that the use of rapid culture-independent diagnostic tests is an essential complement to blood culture for the management of high-risk patients.3
Species Identification. Although the genus Candida includes more than 200 different species, five major species account for 95% to 97% of human infections: C. albicans, C. glabrata, C. krusei, C. parapsilosis, and C. tropicalis. In most populations the incidence of Candida infection is greatest for C. albicans, followed in descending order by C. glabrata, C. parapsilosis, C. tropicalis, and C. krusei. However, the exact distribution may vary by geographic location and risk group.
In addition to the prolonged time to detection inherent in blood cultures, it is also clear that the conventional methods for species identification are cumbersome, often inaccurate, and too slow to provide results within the critical 12- to 24-hour treatment window. Conventional methods for yeast identification include the germ tube test, morphology on chromogenic and cornmeal agar, temperature tolerance, and branded biochemical methods such as those offered by Vitek (bioMérieux), Analytical Profile Index (API; bioMérieux), MicroScan (Beckman Coulter), and others.9 Such tests require isolated colonies and incubation times of 48 to 72 hours before a species identification can be obtained.
It should be noted that the fungal blood culture bottles available for both the BacT/Alert (bioMérieux) and Bactec (Becton Dickinson) blood culture systems are superior to the standard aerobic blood culture bottles for detection of Candida species. This is especially important for the detection of C. glabrata with the Bactec system.
Antifungal Susceptibility Testing. Antifungal resistance is not as prevalent as antibacterial resistance. Nevertheless, the overuse of ineffective or unnecessary antifungal therapies is a driving force for the emergence of antifungal resistance among Candida species, just as the overuse and misuse of antibacterial agents are giving rise to a growing number of antibiotic-resistant bacteria. Indeed, the US Centers for Disease Control and Prevention has specifically noted the increasing incidence of Candida infections due to azole- and echinocandin-resistant strains, and it considers the trend to be a “serious” public health threat that must be addressed through improved use of antifungal agents.
T2MR for the Diagnosis of Invasive Candidiasis
As suggested above, candidemia and other forms of invasive candidiasis—infections involving blood, normally sterile body fluids, and tissues—pose significant diagnostic challenges. In order to provide the best treatment and clinical support, especially in light of the continuing emergence of antimicrobial-resistant pathogens throughout the world, it is increasingly important to accurately detect fungal infections and identify the species causing the infections.
Historically, strategies for the diagnosis of Candida infections have generally relied upon one of three classical laboratory approaches: histopathology, immunology, or microbiology. Newer methods—including biochemical, molecular, proteomic, and radiographic techniques for detecting and identifying pathogenic organisms—have led to valuable tools that can speed therapeutic decisions.
T2 Magnetic Resonance. T2 Magnetic Resonance (T2MR) is a miniaturized, magnetic resonance–based diagnostic approach that measures how water molecules react in the presence of magnetic fields (see Figure 3). T2MR is the first technology that can detect the presence of molecular targets within a sample rapidly and accurately, without the need for time-consuming and labor-intensive purification or extraction of target molecules from the sample.
When compared to molecular diagnostics using nucleic acid extraction with polymerase chain reaction (PCR) for target amplification, the T2MR technology holds a distinct advantage in both speed and limit of detection. While conventional nucleic acid extraction and PCR methods cannot typically detect pathogens below the level of 100 to 1,000 CFU/mL of whole blood, T2MR is able to detect microbes at a density as low as 1 CFU/mL.10 The T2MR method also improves on traditional methods employing PCR by not requiring the extraction of target molecules, a preanalytic step that often results in the loss of significant amounts of the target.
T2MR detection uses magnetic resonance relaxometry to measure the clustering of superparamagnetic particles when their attached probes bind to amplified nucleic acid directly in the sample matrix. T2 Biosystems prepares the superparamagnetic particles during reagent manufacturing by covalently attaching aminated oligonucleotide capture probes to carboxy moieties on the particle surface. This production process utilizes specific nucleic acid sequences to generate particles that will cluster only in response to specific nucleic acid sequences. Presence of the target nucleic acid sequence leads to clustering of the particles and an increase in the T2MR signal.
Because two different capture probes must hybridize to a single nucleic acid target and only ~1×109 copies of nucleic acid are necessary to elicit a detectable change in T2MR signal, the T2MR detection method enables highly specific detection of minute amounts (femtomoles) of nucleic acid in a highly complex background that can include large amounts of non-target nucleic acid, protein, and other biological debris. These attributes of T2MR enable the utilization of a highly efficient assay workflow on the T2Dx instrument to select for freely circulating or white cell-encapsulated intact pathogens. In turn, such selectivity avoids the detection of freely circulating DNA, known as DNAemia, which has been reported to confound test performance. Because the target pathogen is not separated from the original sample matrix, the limit of detection is 1 CFU/mL, and detection at concentrations less than 1 CFU/mL occurs at high probability (70%).10
The T2Candida Panel. Performed on the FDA-cleared and fully automated T2Dx instrument, the T2Candida panel is a rapid diagnostic approach that enables sensitive and specific detection of Candida pathogens directly in whole blood, without the need for culture or nucleic acid extraction steps.11
The T2Candida panel has introduced a new class of infectious disease diagnostics that can rapidly detect and identify the causative pathogen of sepsis directly from a patient blood sample in a culture-independent manner—a significant advance for the rapid and accurate diagnosis of invasive candidiasis. The test enables detection of five species of Candida by category:
- C. albicans and C. tropicalis (A/T)
- C. krusei and C. glabrata (K/G)
- C. parapsilosis (P)
The species groupings are those recommended by the Infectious Diseases Society of America to be used as a surrogate for antifungal susceptibility testing for selecting empiric antifungal therapy.5,6

Figure 4. The T2Candida panel is run by attaching a 4-mL EDTA vacutainer to a T2Dx cartridge, and inserting it into one of the T2Dx drawers.
To obtain results using the T2Candida panel, the operator attaches 4 mL of blood in a “purple top” ethylenediaminetetraacetic acid (EDTA) vacutainer to a T2Candida cartridge and loads it into the T2Dx instrument (see Figure 4). Hands-on time required to initiate processing is typically less than 5 minutes. All assay steps are completed in a fully automated fashion on the T2Dx instrument. Qualitative results are automatically reported on the T2Dx touchscreen user interface, and can also be sent to the laboratory’s information system. Procedural steps that are automated by the T2Dx instrument include:
- Detergent lysis of red and white cells.
- Concentration of cellular debris, intact pathogen cells, and all other solid matrix from 2 mL of the original sample.
- Processing of the concentrated sample matrix with bead beating to lyse pathogen cells.
- Nucleic acid amplification of lysate directly in concentrated sample matrix.
- T2MR detection of amplified products directly in concentrated sample matrix.12
The T2Candida panel is classified as a moderate complexity diagnostic under CLIA. Consequently, performing the test does not require specialist training in either microbiology or molecular biology.
Clinical Trials of the T2Candida Panel
The pivotal clinical trial of the T2Candida panel documented the performance of the panel relative to testing via blood culture.10 The final analysis of the pivotal clinical trial included results from a total of 1,801 patients.
Specifically, 1,501 prospective patients had a sample for blood culture drawn concurrently and from the same anatomical site as the T2Candida sample. In addition, because the investigators anticipated a low prevalence of Candida infections among patients suspected of sepsis—many of whom are so sick that it is difficult to obtain their informed consent—300 additional prospective subjects from the same target population were enrolled and used in the contrived arm of the trial. Of these, samples from 250 patients were seeded with different clinical isolates of the five Candida species at clinically relevant concentrations. Samples from the remaining 50 patients were used as Candida-negative control samples. For all contrived patient samples, concomitant blood cultures obtained prior to spiking were negative.
All samples were analyzed at independent clinical sites in a blinded fashion. The mean time to a result from the T2Candida panel was 4 hours, while obtaining results from blood cultures required at least 120 hours, as the institutional protocol for blood cultures required a 5-day incubation period.
From the trial’s analysis population of 1,801 prospective and contrived subjects, 5,403 T2Candida results were generated (3 results per sample). Assessment of those T2Candida panel results yielded an overall sensitivity of 91.1%, and an overall specificity of 99.4%.
In a follow-on study, investigators calculated the negative predictive value (NPV) of the T2Candida panel among a representative hospitalized population with high-risk characteristics. Accordingly, the NPV for a 5% prevalence of candidemia would be 99.5%.10 A rapid test for candidemia with such a high NPV may prove invaluable to antifungal stewardship efforts.
Additional Studies. In the course of conducting additional studies looking at the performance of the T2Candida panel, a total of 55 patients who were tested using both blood culture and the T2Candida panel were diagnosed as having either candidemia (33 patients) or invasive candidiasis (22 patients). Among the 55 total cases, blood culture was positive in just 33 instances (60%), while the T2Candida panel was positive in 53 instances (96.4%).11 Thus, in this head-to-head comparison with blood cultures drawn at the same time and same anatomic site for the diagnosis of invasive candidiasis, the T2Candida panel detected 22 more Candida patients, and showed a superior sensitivity of 96.4%, versus 60% for blood culture.
In these additional studies, positive T2Candida test results were obtained for 12 proven and 10 probable or possible cases of invasive candidiasis among patients with negative blood cultures.11 Notably, in one patient, 12 sets of blood cultures were negative prior to the diagnosis of intraabdominal candidiasis confirmed by laparotomy and tissue biopsy. The T2Candida result for that patient was obtained 7 days prior to the discovery of the intraabdominal focus of infection. Cases such as this provide striking examples of the potential utility of the T2Candida panel for detecting not only candidemia but also deep-seated candidiasis.
The overall sensitivity per patient of 96.4%, with a mean time to positive species identification of 4.4 hours, is a major advance in the detection of Candida species and the diagnosis of candidemia and invasive candidiasis. The ability to detect and identify the five major species of Candida at levels as low as 1 to 3 CFU/mL may be especially useful in the diagnosis of candidemia from a gastrointestinal source, where the burden of organisms in the bloodstream may be quite low.
Rapid Diagnosis and Patient Outcomes
It is widely understood that the entire diagnostic process for invasive candidiasis is negatively affected by the lack of rapid, sensitive, and minimally invasive diagnostic tests. Despite improvements in blood culture technology, the time to detection of yeasts using automated blood culture methods averages 3 to 5 days, with additional time required for identification of Candida to the species level.
Recognition of such imperfections in the diagnostic process, coupled with an awareness of the potential harms associated with delays in the treatment of invasive candidiasis, has prompted many clinicians to initiate an empirically selected course of antifungal therapy prior to identification of a yeast in patients considered to be at high risk for candidemia and other forms of invasive candidiasis. This practice has been shown to be largely ineffective in reducing the morbidity and mortality associated with invasive candidiasis. Moreover, it results in excessive costs to the hospital and increased selection pressure for resistance to both azole and echinocandin antifungal agents.
With T2Candida, the only diagnostic test cleared by the FDA for blood culture-independent Candida species identification from whole blood samples, new possibilities exist for the early diagnosis and management of invasive candidiasis in high-risk patients. A potential strategy for use of the T2Candida panel for diagnosis of invasive candidiasis is to stratify patients according to risk and conduct prospective screening using the rapid test coupled with other diagnostic modalities (eg, blood cultures, imaging studies). Another potential strategy may enable rapid antibiotic susceptibility measurements by guiding the selection and sampling of blood cultures prior to positivity for subsequent analysis based on a positive T2Candida panel result.
Adoption of such strategies should facilitate earlier species-level diagnosis, thereby facilitating initiation of targeted preemptive antifungal therapy. In turn, such practices should result in a decrease in Candida-associated morbidity, mortality, and the duration of hospitalization. A highly sensitive and specific test such as the T2Candida panel should also help to reduce the use of empirical therapy, with concurrent reduction in selection pressure for resistance as well as cost savings for the hospital.
Michael A. Pfaller, MD, is chief medical officer, and Thomas J. Lowery, PhD, is chief scientific officer, at T2 Biosystems, Lexington, Mass. For further information, contact CLP chief editor Steve Halasey via [email protected].
References
- Pfaller MA, Diekema DJ. Epidemiology of invasive candidiasis: a persistent public health problem. Clin Microbiol Rev. 2007;20(1):133–163.
- Vincent JL, Rello J, Marshall J, et al. International study of the prevalence and outcomes of infection in intensive care units. JAMA. 2009;302(21):2323–2329; doi: 10.1001/jama.2009.1754.
- Pfaller MA, Castanheira M. Nosocomial candidiasis: antifungal stewardship and the importance of rapid diagnosis. Med Mycol. 2016;54(1):1–22; doi: 10.1093/mmy/myv076.
- Morrell M, Fraser VJ, Kollef MH. Delaying the empiric treatment of candida bloodstream infection until positive blood culture results are obtained: a potential risk factor for hospital mortality. Antimicrob Agents Chemother. 2005;49(9):3640–3645.
- Castanheira M, Messer SA, Rhomberg PR, Pfaller MA. Antifungal susceptibility patterns of a global collection of fungal isolates: results of the SENTRY antifungal surveillance program (2013). Diagn Microbiol Infect Dis. 2016;85(2):200–204; doi: 10.1016/j.diagmicrobio.2016.02.009.
- Pappas PG, Kauffman CA, Andes DR, et al. Clinical practice guideline for the management of candidiasis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis. 2016;62(4):e1–50; doi: 10.1093/cid/civ933.
- Clancy CJ, Nguyen MH. Finding the “missing 50%” of invasive candidiasis: how nonculture diagnostics will improve understanding of disease spectrum and transform patient care. Clin Infect Dis. 2013;56(9):1284–1292; doi: 10.1093/cid/cit006.
- Avni T, Leibovici L, Paul M. PCR diagnosis of invasive candidiasis: systematic review and meta-analysis. J Clin Microbiol. 2011;49(2):665–670; doi: 10.1128/jcm.01602-10.
- Jorgensen JJ, Pfaller MA, Carroll KC, et al., eds. Manual of Clinical Microbiology. 11th ed. Washington DC: ASM Press, 2015.
- Mylonakis E, Clancy CJ, Ostrosky-Zeichner L, et al. T2 magnetic resonance assay for the rapid diagnosis of candidemia in whole blood: a clinical trial. Clin Infect Dis. 2015;60(6):892–899; doi: 10.1093/cid/ciu959.
- Pfaller MA, Wolk DM, Lowery TJ. T2MR and T2Candida: novel technology for the rapid diagnosis of candidemia and invasive candidiasis. Future Microbiol. 2016;11(1):103–117; doi: 10.2217/fmb.15.111.
- How to conduct the test [online]. Lexington, Mass: T2 Biosystems, 2016. Available at: www.t2biosystems.com/t2candida/how-to-conduct-test. Accessed January 3, 2017.








I’m not affiliated with any company. Could you tell me if this type of testing is administered in Texas anywhere? It would be of desperate and great help.
Where can I go to get tested for this around southern California